Blog
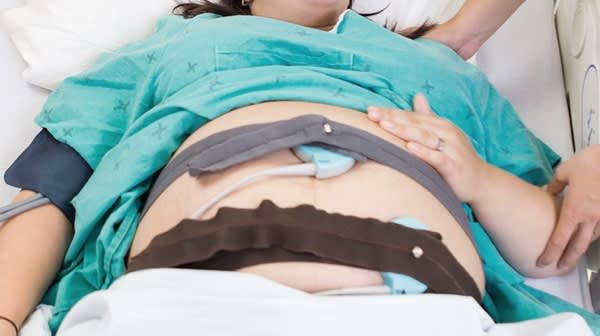
Pain Relief During Labour
Thursday 13th July 2017
Giving birth is a unique experience and it’s impossible to predict how you will feel physically. Some level of discomfort is to be expected but if things go beyond your expectations, it’s reassuring to know pain relief is available. Understanding different methods of pain relief and when they might be administered should make your labour more bearable.
TENS machine
Prevents pain signals from reaching your brain
Especially effective in the first stages of labour
Helps your body release ‘feel-good’ endorphins
Can be controlled to match pain levels
No known effects on the baby
TENS machines are widely available for hire online and from chemists − make sure you get a machine specifically designed for use in pregnancy, not just for general pain relief. It can take about an hour before you really feel the benefits – so start using it as soon as you go into labour. It can also help soothe backache towards the end of pregnancy.
Gas and air
- A mixture of air and nitrous oxide (laughing gas)
- Can quickly reduce the pain of contractions
- Can make your mouth a little dry and cause nausea while inhaling
- No known effects on the baby
Sometimes known as Entonox, gas and air is administered orally and can be used at home, during births or combined with other pain relief. To feel the effect when you really need it, inhale as soon as you get a contraction.
Water
Even if you don’t want a water birth, warm water (kept at around body temperature), can help you relax and soothe painful contractions. Most birthing suites have a birth pool or shower room, so ask your midwife if you can have a bath or stand (sit or squat!) under a warm running shower.
Intramuscular injection
- Helps to take the edge off pain rather than removing it
- Helps you feel more relaxed – you may be able to sleep in-between contractions
- Needs about 20 minutes to take effect and can last 2–4 hours
- Can make you feel sick
Can make the baby drowsy and interfere with its breathing and initial breastfeeding
This method of pain relief involves injecting a drug, such as pethidine or diamorphine, into your thigh or buttock. As it can make you nauseous, it’s often given with an anti-sickness drug at the same time. Due to the possible side effects on your baby, it is not usually given if your midwife thinks you will deliver quickly. And if you are still feeling the effects towards the end of labour, you may find it more difficult to push.
Epidural
- A local anaesthetic injected into the lower back
- Has a timed or controlled release
- Takes pain away and leaves you with a clear head to focus on labour
- Has very few complications but can cause side effects such as shivering, low blood pressure and, in rare cases, bad headaches
Epidurals are only available at hospitals and are usually administered once the cervix is dilated to around 5 or 6cm and there are strong contractions. This type of traditional epidural will leave you with no feeling in your legs, so you’ll be bed-bound and may need help timing your pushes during the delivery.
Mobile epidurals
Most hospital units now use mobile epidurals – also known as walking epidurals. Unlike the more traditional epidurals, mobile epidurals leave you with some feeling in your legs and perineal area, so you are more able to sense when to push.
Whatever your pain relief preference, always discuss the options with your midwife and remember to check that your hospital provides the option you want.
NEXT STEPS
- If you’re planning a home birth, ask your midwife about the types of pain relief available to you.
- If it’s a hospital birth, ask if there will be a bath or shower readily available
- Ensure you include your pain relief preferences in your birth plan





